Did you know that 99.9% of your DNA is identical to everyone else’s (1)? Although human genetic make-up is similar, vast differences exist between the microbes that inhabit our bodies – termed the microbiome. A particularly diverse community of microbes inhabit your intestines and are known as the gut microbiome. Shaped by biological, genetic, and environmental factors, the microorganisms that inhabit our guts differentiate us from others and have many roles in both health and disease. This blog will discuss the diversity of the human gut microbiome, and some of the ways in which it helps and hinders us.
So, what is the gut microbiome?
Living within your gut is an intricate and extensive community of microbes, including bacteria, viruses, archaea, fungi, and protozoans (2). You may have heard the terms ‘microbiota’ and ‘microbiome’ used interchangeably, but they actually have slightly different meanings.
- Microbiota – this term refers to the entire population of microorganisms present in your gut. You can think of this as ‘who is there?’ (3).
- Microbiome – this term refers to the microbiota (who is there?) as well as their genetic material (what can they do?) and metabolic functions (what are they doing?) (3).
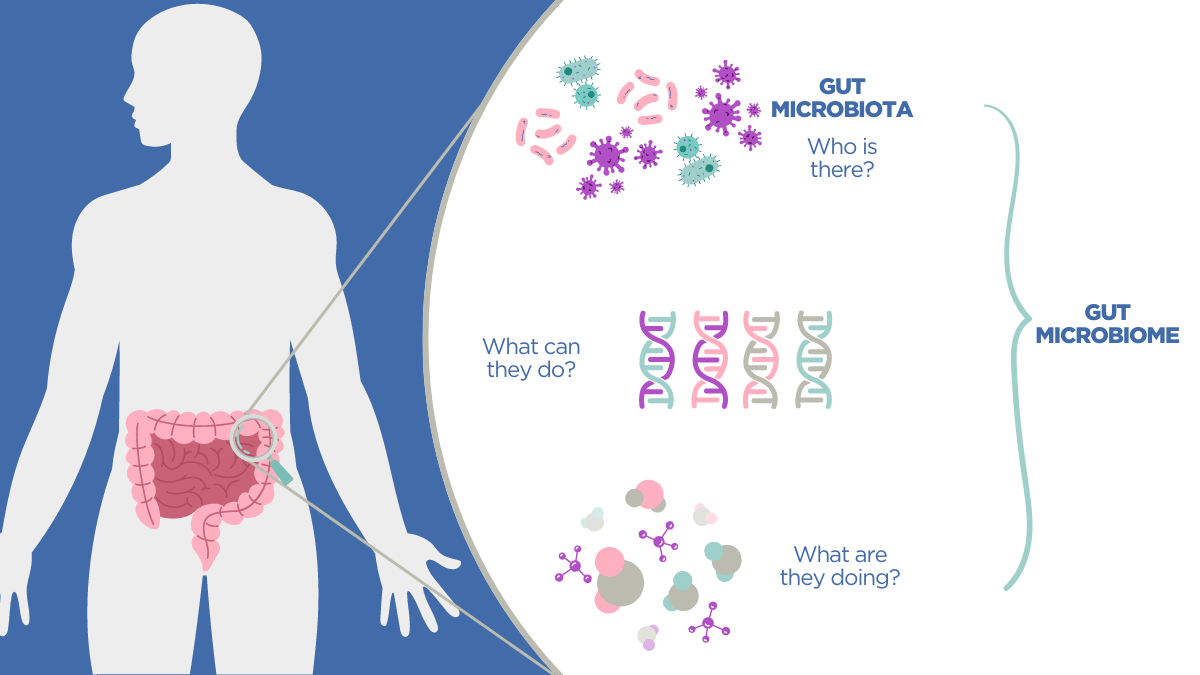
We’ll use the term ‘gut microbiome’ throughout this blog, and will primarily discuss gut bacteria, the largest and best studied component of your gut microbiome. Rough estimates suggest that your gut may contain up to 1000 bacterial species and 2 million bacterial genes – that’s 100 times the number of genes you have (around 20,000) (4). Despite your high genetic similarity to other humans, your gut microbiome is more unique and can be 80-90% different from someone else’s (4). So that answers what the microbiome is, but what does the microbiome do?
What shapes my gut microbiome?
When born, babies are exposed to the world of microbes around them, acquiring some of their mother’s bacteria if delivered vaginally as well as benefiting from the microbes present in breast milk if breast fed (5). Once exposed to solid foods, their gut microbiomes enter the next phase of growth. By the age of three, children’s microbial composition tends to reflect that of their cultural circles, resembling their family’s most closely (6). As we grow, the gut microbiome is molded by a combination of genetics (7), diet, and geographical location (8).
Gut Microbiome Diversity
A study comparing children in urban Italy and rural Burkina Faso found that the African children had significantly more short-chain fatty acid (SCFA) producing bacteria (9). SCFAs are produced from breaking down undigestible fibers into a form that the body can absorb as energy. Children in Burkina Faso also had several additional species that were not found in the Italian children. These microbes contained specific genes to break down plant fibers, enabling the children to extract additional extra calories from the foods they ate. SCFAs also promote immunity and other aspects of our health, as explained in the section on micronutrients below. Since the typical Western diet is less rich in plant fibers, more homogenous and higher in processed foods, it is unsurprising that the European children had less microbial richness and biodiversity.
However, research suggests that the gut microbiome can switch rapidly in response to changing diet, illness, medications or physiological conditions such as high altitude (8). Sometimes, changing conditions can cause temporary gut disruption such as when someone experiences traveler’s diarrhea. Yet, slowly incorporating locally grown foods into your diet could help boost microbiome diversity. Now we know what influences the gut microbiome, but what does it do?

What does the gut microbiome do?
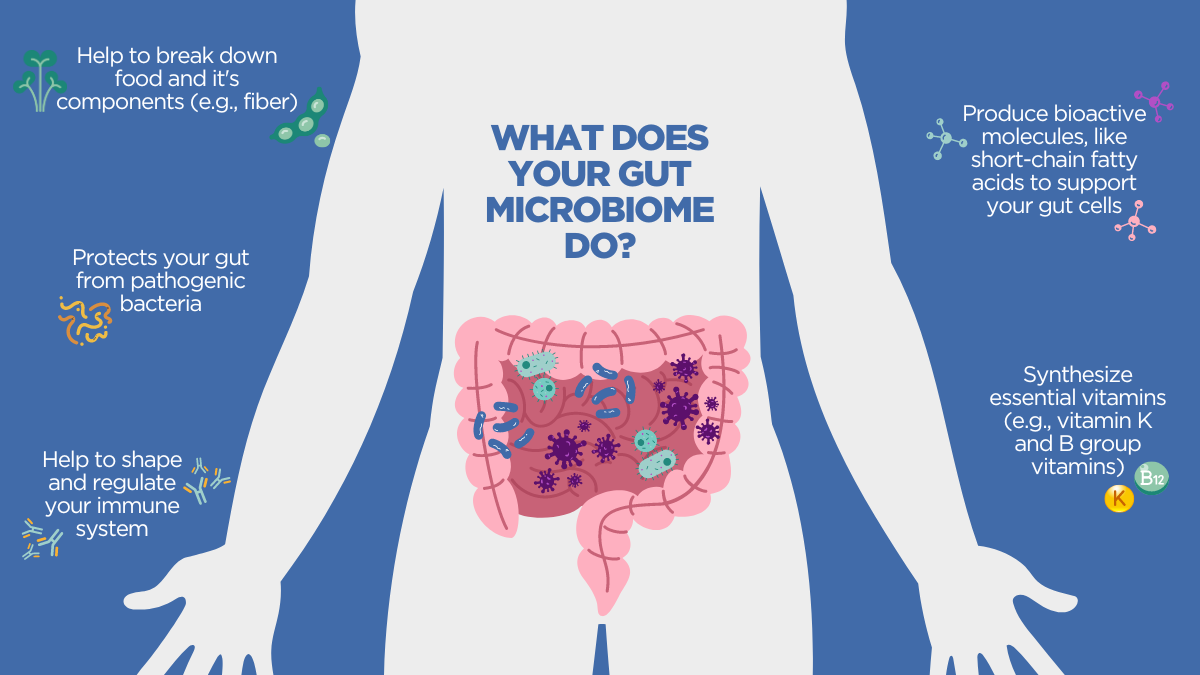
Despite its microscopic constituents, your gut microbiome is one of your biggest supporters, with a diverse set of roles as a result of human and microbial co-evolution. Your gut microbiome contributes to food breakdown, micronutrient production, protection from invading bacteria, and even helps to shape your immune system. So your microbiome does a lot! Let’s explore these roles in a little more depth.
Food breakdown
Your body is responsible for most digestive processes, producing enzymes to break down fats, carbohydrates, and proteins. However, one component of foods – fiber – cannot be broken down by your enzymes and needs input from your gut microbes (2). In the large intestine, your gut bacteria work to digest the fiber you consume, using their own arsenal of enzymes (2). Fiber acts as food for your gut microbes, so it’s important that you consume the recommended intake (~30g per day) to ensure that you are providing them with the fuel they need to thrive.
Micronutrient and beneficial molecule production
In the process of breaking down fiber, your gut microbes produce an array of bioactive molecules. Short-chain fatty acids (SCFAs; propionate, butyrate, and acetate) are one such class of molecules. SCFAs can benefit your gut in many ways, including reducing inflammation, providing fuel for cells in your colon, and impacting the speed at which food travels through your intestine (10)
Your gut bacteria can also synthesize essential vitamins, notably vitamin K and B group vitamins such as biotin, folate, and thiamine. In fact, for several B group vitamins (cobalamin, folate, niacin, pyridoxine), gut bacteria are estimated to contribute more than 25% of your daily recommended intake (11).
Protection from harmful bacteria and immune system support
In addition to synthesizing valuable compounds and vitamins, bacteria in your gut can also provide protection against invading pathogens that might be harmful to our health like E. coli, Salmonella, and Campylobacter species (12). By producing specific metabolites, gut bacteria induce the synthesis of antimicrobial proteins by gut cells to help stop microbial infections from taking hold. Additionally, the presence of a normal, healthy gut microbiome can hinder the establishment of intestinal pathogens – a phenomenon called ‘colonization resistance’ (12).
Gut microbes also have roles in shaping and regulating your immune system, especially during infancy. Interactions between your gut microbiome and your immune system are complex and dynamic, and much of the research exploring this connection is carried out in germ-free mice (mice without gut microbes) (13). In germ-free mice, a lack of gut microbiome has resulted in intestinal tissue defects, reduced levels of immune cells, and reduced immune function (13), highlighting the important of the gut microbiome in supporting the immune system.
The gut microbiome in health and disease
There are numerous reports of the gut microbiome being involved in disease states. Although much of the research in this area is promising, many of the relationships between gut microbes and human disease are associative, meaning that we don’t know if the gut microbiome is driving the disease state or if the disease causes changes to the gut microbiome (14). Nevertheless, a growing body of literature has identified relationships between gut microbes and obesity, mental health, nutrition-related diseases, cancer, and cardiometabolic diseases. We will explore the connections between the gut, its microbial inhabitants, and human disease further in future blogs.
Is it important to know what’s in your gut microbiome?
Discussing the role of gut microbiome poses a question – do we need to know ‘who is there’? Although results from gut microbiome tests can be interesting, research hasn’t yet identified strong causative links between gut microbes and disease, so it can be challenging to make useful inferences from gut microbiome testing.
Additionally, knowing about the community structure at a single time point (what many microbiome testing kits offer) provides very little practical insight, given that the gut microbiota can change substantially in response to diet in as little as 24 hours (10). What is useful, is looking at microbial metabolites i.e. the compounds produced by your gut microbiome, as these can give an indication on your overall health. Our in-clinic breath test, OMED Health Inside Insights, offers a deep dive into the presence of a wide array of compounds including SCFAs on your exhaled breath. The test also looks at compounds related to your metabolic health and pollution exposure. You can discover more here.
For most people, focusing on habits that promote gut microbiome health, such as eating a diversity of plant foods, reducing stress, getting plenty of sleep, and exercising regularly, is the best way to support your gut microbiome, so they can support you in return.
We can help you to take control of your gut health
If you are living with uncomfortable digestive symptoms, Gut Reset+ can help to identify whether your gut microbiome is hindering rather than helping you. You can also purchase your OMED Health Breath Analyzer and App which can aid in the diagnosis of small intestinal bacterial overgrowth (SIBO) and Intestinal Methanogen Overgrowth (IMO), find out your triggers, and monitor whether your personalized treatment pathway is working.
References
- Genetics vs. Genomics Fact Sheet. Genome.gov. Published September 14, 2022. Accessed May 15, 2023. https://www.genome.gov/about-genomics/fact-sheets/Genetics-vs-Genomics
- Jandhyala SM, Talukdar R, Subramanyam C, Vuyyuru H, Sasikala M, Reddy DN. Role of the normal gut microbiota. World J Gastroenterol. 2015;21(29):8787-8803. doi:10.3748/wjg.v21.i29.8787
- Berg G, Rybakova D, Fischer D, et al. Microbiome definition re-visited: old concepts and new challenges. Microbiome. 2020;8(1):103. doi:10.1186/s40168-020-00875-0
- Gilbert JA, Blaser MJ, Caporaso JG, Jansson JK, Lynch SV, Knight R. Current understanding of the human microbiome. Nat Med. 2018;24(4):392-400. doi:10.1038/nm.4517
-
Notarbartolo V, Giuffrè M, Montante C, Corsello G, Carta M. Composition of Human Breast Milk Microbiota and Its Role in Children’s Health. Pediatric Gastroenterology, Hepatology & Nutrition [Internet]. 2022 May 1 [cited 2025 Jun 17];25(3):194–210. doi:10.5223/pghn.2022.25.3.194
-
Yatsunenko T, Rey FE, Manary MJ, Trehan I, Dominguez-Bello MG, Contreras M, et al. Human gut microbiome viewed across age and geography. Nature [Internet]. 2012 Jun [cited 2025 Jun 17];486(7402):222–7. Available from: https://doi.org/10.1038/nature11053
-
Goodrich JK, Waters JL, Poole AC, Sutter JL, Koren O, Blekhman R, et al. Human Genetics Shape the Gut Microbiome. Cell [Internet]. 2014 Nov 6 [cited 2025 Jun 17];159(4):789–99. doi: 10.1016/j.cell.2014.09.053
-
Patel PG, Patel AC, Chakraborty P, Gosai HB. Impact of Dietary Habits, Ethnicity, and Geographical Provenance in Shaping Human Gut Microbiome Diversity. In: Kothari V, Kumar P, Ray S, editors. Probiotics, Prebiotics, Synbiotics, and Postbiotics: Human Microbiome and Human Health [Internet]. Singapore: Springer Nature; 2023 [cited 2025 Jun 17]. p. 3–27. doi: 10.1007/978-981-99-1463-0_1
-
Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa [Internet]. [cited 2025 Jun 17]. doi: 10.1073/pnas.1005963107
- Blaak EE, Canfora EE, Theis S, et al. Short chain fatty acids in human gut and metabolic health. Benef Microbes. 2020;11(5):411-455. doi:10.3920/BM2020.0057
- Rowland I, Gibson G, Heinken A, et al. Gut microbiota functions: metabolism of nutrients and other food components. Eur J Nutr. 2018;57(1):1-24. doi:10.1007/s00394-017-1445-8
- Iacob S, Iacob DG, Luminos LM. Intestinal Microbiota as a Host Defense Mechanism to Infectious Threats. Frontiers in Microbiology. 2019;9. Accessed May 15, 2023. https://www.frontiersin.org/articles/10.3389/fmicb.2018.03328
- Zheng D, Liwinski T, Elinav E. Interaction between microbiota and immunity in health and disease. Cell Res. 2020;30(6):492-506. doi:10.1038/s41422-020-0332-7
- Witkowski M, Weeks TL, Hazen SL. Gut Microbiota and Cardiovascular Disease. Circulation Research. 2020;127(4):553-570. doi:10.1161/CIRCRESAHA.120.316242
- Sonnenburg JL, Bäckhed F. Diet–microbiota interactions as moderators of human metabolism. Nature. 2016;535(7610):56-64. doi:10.1038/nature18846